This week, Thyroid School is covering some of the common root causes behind hypothyroidism including poor overall production and conversion. It’ll take a few weeks to review them all, so hang in there with me!
Last email, I discussed “step one” to figuring out your major root cause(s)— differentiating between whether it is autoimmune or not autoimmune.
If you DID identify antibodies, you may have a condition called Hashimoto’s, which is the most common cause of hypothyroidism in the U.S.— definitely talk with your doctor about whether that diagnosis fits you! It may not change your course of medication management, but your diet and lifestyle management will be a tad bit different.
Regardless of whether or not autoimmunity is your root cause, you’ll want to pay attention to this email as it applies to both root causes. The production of thyroid hormone is a nutrient dependent process to say the least. We learned in past Thyroid School emails that the thyroid is the thermostat of the body that increases and decreases depending on messages it gets from the brain. Stressed? Down goes the thyroid. Under eating? Down goes the thyroid.
The production of thyroid hormones relies heavily on iron, tyrosine (an amino acid), iodine, selenium, B-Vitamins, Vitamin D, Vitamin C, and Vitamin E. With this list alone, you can see why simply focusing on calories and macros alone isn’t enough to ensure proper nutrient density— after all, 100 calories of kale and 100 calories of sugar will send very different messages to the body. For this reason, I often suggest optimizing the diversity and nutrient density of your food BEFORE tackling calorie and macro-nutrient counting. (This may be shocking to you if you’ve always heard otherwise, but trust me on this one!)
While the thyroid produces 4 main thyroid hormones (T1, T2, T3, and T4), let’s focus in on the most abundant first— T4. (Don’t worry, I’ll discuss T3 A LOT soon. Additionally, T1 and T2 are less bioactive, so I won’t cover those as much!)

What does it take to produce T4? A LOT of nutrients! Your body is like a business in the sense that it “takes money to make money”. In order to produce energy, hormones, metabolize, and have basic bodily functions, etc., the body requires a tremendous number of vitamins, minerals, amino acids, and fatty acids to get the job done. Some are produced endogenously (inside the body) while the majority of them must be obtained through food. This is a big reason that undernourishment is a predisposing factor for hypothyroidism. Fewer nutrients available = less fuel to make hormones.
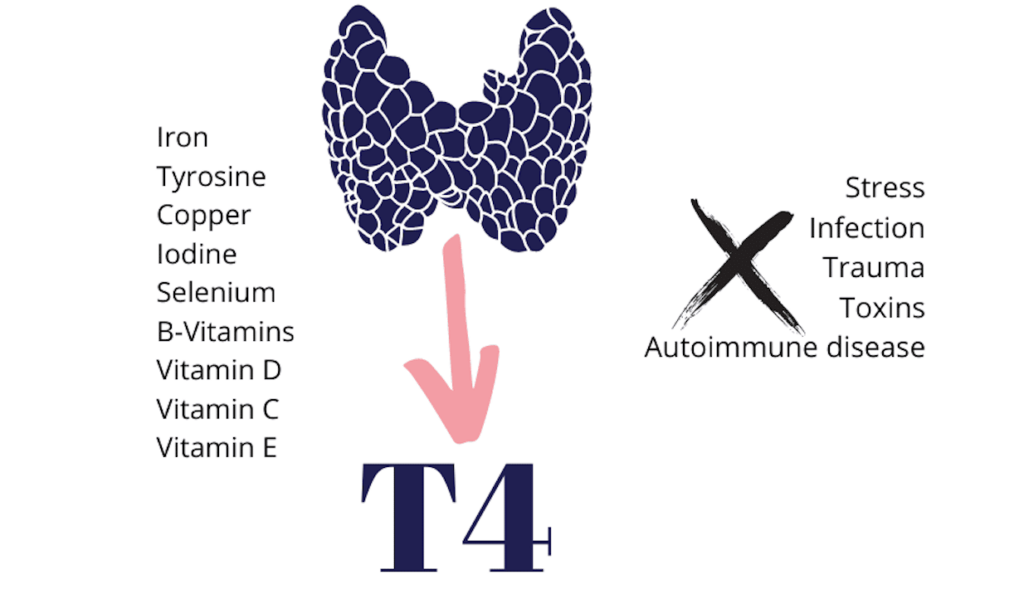
Nutrient spotlights below
Iron: the “heme” (or blood) form of iron is found in animal proteins. Heme iron is much more bioavailable and the form that humans use most efficiently. “Non-heme” iron found in leafy greens and beans is not used as readily and is often present in competing nutrients, like calcium and oxalates, that hinder the absorption. This is one of the main reasons I do not suggest vegan and/or vegetarian diets as it can induce and/or worsen hypothyroidism. Iron deficiency in and of itself is a big risk factor for hypothyroidism. That said, iron balance is delicate and iron supplementation should not be taken lightly. Nowadays, we have so much exposure to iron through food fortification, but we are dealing with more iron deficiency than ever. Why is that? (Keep reading to find out!) Iron is SO important in the body that we actually have a built-in “recycling” system for it. Before you jump straight to supplements, you’ll definitely want to optimize the nutrient cofactors like Vitamin A, copper, zinc, magnesium, Vitamin C (to name a few) and also test a full iron panel (ferritin, serum iron, TIBC, transferrin, and % transferrin) to determine if you really do need iron supplementation. Iron supplements can cause oxidation (think of this as an imbalance between inflammation and antioxidants) in the body when taken unnecessarily. Best food sources: animal proteins, liver/organ meats, eggs, and cooking cast iron skillet; you can also increase absorption by having iron-rich foods alongside Vitamin A, Vitamin C
Tyrosine: this is an amino acid (think building blocks of protein) that is considered a “conditionally essential” amino acid. Essential amino acids are those that we must get through our diet, while non-essential amino acids are typically produced in the human body. Amino acids can become “conditionally essential”– meaning it needs to be obtained through the diet despite it being produced in the body. Common circumstances for this include inherited genetic disorders in which production is impaired. Additionally, if demand for a particular amino acid is very high in response to internal supply, then the amino acid must be consumed through diet. Tyrosine is produced endogenously (or internally) from phenylalanine (an essential amino acid). The conversion of phenylalanine into tyrosine requires nutrient cofactors including Vitamin B6, folate, and copper. Supporting optimal tyrosine levels means including the foods that are high in tyrosine and phenylalanine as well as folate (“foliage”//leafy greens), copper (shellfish, oysters, liver), and Vitamin B6 (nuts, seeds, meats)
Copper: Copper is the third most abundant mineral in the body and plays an important role in the production of thyroid hormone in the body. It balances with calcium to help prevent over-absorption of T4 into the cells. Copper and iron also need to be balanced with each other because copper deficiency can lead to iron deficiency. Copper deficiency can result from poor intake of copper-rich foods, but also from prolonged zinc supplementation (ALERT: for all of you pounding down the zinc since the pandemic started! We need zinc, but need to be sure it is balanced with copper food sources!!) Copper-rich foods include beef liver, shellfish, bee pollen, and cacao.
Iodine: as previously discussed, iodine deficiency is a common cause of hypothyroidism in underdeveloped countries. T4 is produced by combing iodine with tyrosine. While iodine deficiency has decreased since iodization of salt in the 1920s, some contributing factors to lower levels include: poor soil quality, other nutrient deficiencies (like Vitamin A, iron, and selenium), as well as increased demand (like during pregnancy). Iodine balance is important because too much can be problematic, especially for autoimmune hypothyroid. I’ll be sure to discuss this in future emails, but long story short, over supplementation with iodine without proper supply of other antioxidants (selenium, Vitamin E, and Vitamin A, for example) can lead to a build up of hydrogen peroxide in the body. Hydrogen peroxide is a normal byproduct of iodine conversion that is normally neutralized by antioxidants, but if those antioxidants aren’t available, you can actually be doing a lot more harm than good with those iodine supplements!
Selenium: selenium is a mineral found in soil most well known for the conversion of inactive to active thyroid. However, it also lends a helping hand to overall thyroid hormone production as well as serving as a precursor to important antioxidants and selenoproteins. Antioxidants are important because the process of producing thyroid hormone can have some inflammatory effects if nutrients aren’t well balanced. (Okay, don’t freak out just yet! This mostly happens from blind supplementation or greatly over consuming high iodine foods without also including selenium). Selenium and iodine balance must be maintained because too much iodine relative to selenium can lead to a build up of hydrogen peroxide in the body. Foods highest in selenium include Brazil nuts, animal proteins, beef liver, seafood, and whole grains.
Vitamin D: Vitamin D is a fat-soluble vitamin that regulates immune function, inflammatory molecules, hormone status, glucose regulation, and several other metabolic functions in the body. Vitamin D is most notably obtained through sun exposure, but can also be supported through consumption of fatty fish (like salmon). Vitamin D deficiency is very common which can be related to poor sun exposure, high demand (due to inflammation and immune dysregulation), as well as other deficiencies including Vitamin A and Magnesium deficiency.
Vitamin C: Vitamin C is found most in fresh fruits and vegetables. Cooking at high heat as well as boiling can decrease the bioavailability of Vitamin C. This doesn’t mean that you have to transition to an all “raw foods” diet, as cooking can also unleash other vitamins and minerals! Vitamin C is important for iron absorption and utilization, tissue integrity, and balancing the immune system. Some studies have even shown that Vitamin C supplementation can regulate thyroid antibody levels. Fun fact: Vitamin C deficiency was common in sailors because of poor access to fresh fruits and vegetables, so they began to make sauerkraut and other fermented foods as a means to support their Vitamin C levels.
Vitamin E: Vitamin E is another fat-soluble vitamin crucial for thyroid hormone production. It has antioxidant effects that help to regulate inflammation and immune function. It works synergistically with selenium and iodine. Vitamin E can be found in nuts, seeds, and green leafy vegetables.
B-Vitamins: B-vitamins are energy-producing vitamins that act as fuel for most metabolic activity. We get B-Vitamins from animal proteins, nuts, seeds, beans, and leafy greens. Additionally, we can produce certain B-Vitamins in our GI tract. Vitamin B12 deficiency, specifically, is common among those with hypothyroidism. There are several reasons for deficiency of B12 including autoimmunity, poor stomach acidity (common in hypothyroid), and poor absorption in the gut (also common in hypothyroidism).
Lots of information here! Try not to get overwhelmed.
Start here: focus on improving the quality of your food away from highly processed to more whole-food form. This doesn’t mean NO processed foods ever, but rather transitioning from worrying about calories and macros (for now) to nutrient density.
Hate liver and other organ meats? Ugh, me too!! Personally, I take Ancestral Nutrition supplements to bridge the gap. (This is NOT a personalized recommendation nor am I affiliated with this company, I just like their products!)
How do you know what nutrients you need? TEST, don’t guess! We can help w/ that!
Disclaimer: Please note that “Thyroid School” emails from Chews Food Wisely, LLC (and Nicole Fennell, RD) are not intended to create any physician-patient relationship or supplant any in-person medical consultation or examination. Always seek the advice of a trained health professional with any questions you may have regarding a medical condition and before seeking any treatment. Proper medical attention should always be sought for specific ailments. Never disregard professional medical advice or delay in seeking medical treatment due to information obtained in “Thyroid School” emails. Any information received from these emails is not intended to diagnose, treat, or cure. These emails, websites, and social media accounts are for information purposes only. The information in these emails, websites, and social media accounts are not intended to replace proper medical care.

EMAIL:
hello@chewsfoodwisely.com
VIRTUAL APPOINTMENTS ONLY
Business Mailing Address:
2525 Robinhood Street
Houston, Texas 77005
© 2026 Chews Food Wisely. All Rights Reserved. Website Designed by AVM
Disclaimers | Privacy Policy | Terms of Purchase | Terms and Conditions